 Secondary outcomes included gas exchange other than PaCO 2 24 h after randomisation, inspiratory effort, dyspnoea, consciousness, NPPV tolerance, patient–ventilator asynchrony, cardiac function, ventilator-induced lung injury (VILI), and NPPV-related adverse events. The primary outcome was PaCO 2 24 h after randomisation. 
In this physiological, randomised controlled trial, we assigned 24 AECOPD patients to undergo either high-intensity NPPV ( n = 12) or low-intensity NPPV ( n = 12). 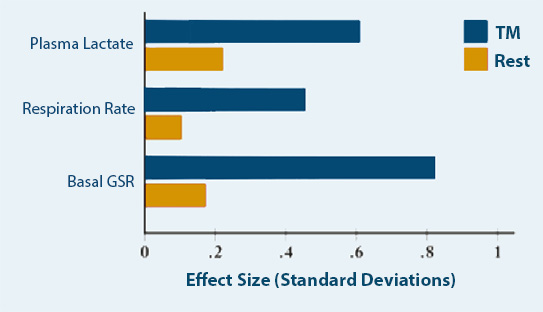
We tested whether high-intensity NPPV is more effective than low-intensity NPPV at decreasing PaCO 2, reducing inspiratory effort, alleviating dyspnoea, improving consciousness, and improving NPPV tolerance in patients with acute exacerbation of chronic obstructive pulmonary disease (AECOPD). High-intensity noninvasive positive pressure ventilation (NPPV) is a novel ventilatory approach to maximally decreasing elevated arterial carbon dioxide tension (PaCO 2) toward normocapnia with stepwise up-titration of pressure support. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
